Q1Medicare.com - Medicare Prescription Drug Plans: FAQs
Newest FAQs
-
May, 08 2024 — It depends on your financial status. If you have been approved for financial "Extra Help" with your Medicare Part D expenses (and have had no changes in your finances), you will not need to re-a . . .
-
May, 06 2024 — A Special Enrollment Period (SEP) allows a Medicare beneficiary to join, switch, or drop their Medicare Part D prescription drug plan (PDP) or Medicare Advantage plan (MA or MAPD) outside of the ann . . .
-
May, 06 2024 — Maybe, depending on your situation. Most people cannot change their stand-alone Medicare Part D plan coverage after the December 7th annual Open Enrollment Period (AEP) deadline. And Medi . . .
-
May, 05 2024 — If your drug plan has both preferred and standard network pharmacies, you probably will pay less for your formulary prescription drugs when using one of your plan’s preferred network pharmacies.
-
May, 05 2024 — If you are eligible for Medicare and you don't have drug coverage through your employer, VA, or other source, additional prescription drug coverage is available to you through either: (1) a stand-a . . .
-
May, 04 2024 — Probably not. In some situations, you have the right to ask your Medicare Part D prescription drug plan to move a higher-costing drug to a lower-costing formulary tier. However, usually such a "tiering exception" is not available for plans with only one Specialty Drug
-
May, 02 2024 — Yes, in some situations you have the right to ask your Medicare prescription drug plan to move a formulary medication to a lower-costing formulary tier. But, you cannot reduce the cost of a Tier 5 Specialty drug, nor can you reduce the cost of a now-covered, non-formulary drug.
-
May, 02 2024 — No. A Medicare Part D plan will not allow you to request a tiering exception for a drug (moving a drug to a lower-costing formulary tier) when your plan has just approved your formulary exception request to cover the non-formulary drug.
-
May, 02 2024 — The cost of covering a non-formulary drug will depend on your Medicare drug plan. Your Medicare Part D plan has some flexibility with regard to what you will pay for the coverage of a non-formul . . .
-
May, 02 2024 — A formulary exception is a type of coverage determination request whereby a Medicare plan member asks their Medicare Part D plan to cover a non-formulary drug or amend the plan's usage management restrictions that are placed on the drug.
-
May, 02 2024 — Ask for a transition fill of your existing non-formulary drug, check for alternative drugs or generics covered by your Medicare drug plan, ask for a formulary exception covering the non-formulary drug, appeal any negative decisions, and finally use a Drug Discount card.
-
 Apr, 30 2024 — Maybe. Even with the 75% Donut Hole discount, you may find that you are paying more for your formulary drugs when you leave your Initial Coverage Phase and enter the Coverage Gap - depending on whether or not you were paying less than 25% of retail in your Initial Coverage Phase.
Apr, 30 2024 — Maybe. Even with the 75% Donut Hole discount, you may find that you are paying more for your formulary drugs when you leave your Initial Coverage Phase and enter the Coverage Gap - depending on whether or not you were paying less than 25% of retail in your Initial Coverage Phase. -
Apr, 24 2024 — Maybe. This particular Special Enrollment Period (SEP) is exceptional, and will only be granted if the changes to your provider network are considered as "significant". In addition, you cannot simply . . .
-
Apr, 23 2024 — Yes. If you use a Special Enrollment Period (SEP) to change Medicare drug plans during the year, you will find that both the total retail value of your drug purchases and the total value of your out-of-pocket spending (TrOOP) transfer to your new Part D plan.
-
Apr, 23 2024 — Yes. Medicare Part D prescription drug plans (PDPs and MAPDs) are required to keep track of each person’s prescription drug spending or TrOOP costs - so your out-of-pocket spending and . . .
-
Apr, 23 2024 — If you use a Special Enrollment Period to change Medicare Part D drug plans during the year, your drug purchase history moves with you to your new Medicare plan. So if you are in the Donut Hole and move to another Part D plan, most likely you will still be in the Donut Hole.
-
Apr, 23 2024 — Maybe. If you are able to change or transfer to another Medicare Advantage plan offered by the same company during the plan year, you may be able to transfer the amount that you have spent for your Medicare Part A and Part B coverage toward your new plan's MOOP limit.
-
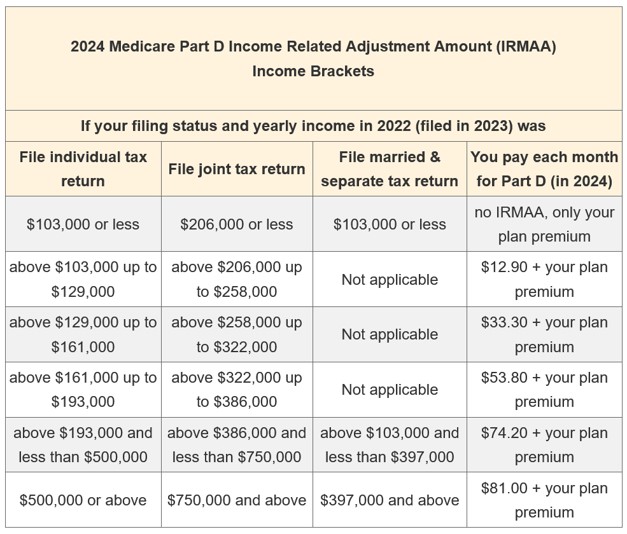 Apr, 20 2024 — If you are a Medicare beneficiary with higher annual earnings, you may be assessed an Income-Related Monthly Adjustment Amount (or IRMAA) which is an additional amount that you pay together with your . . .
Apr, 20 2024 — If you are a Medicare beneficiary with higher annual earnings, you may be assessed an Income-Related Monthly Adjustment Amount (or IRMAA) which is an additional amount that you pay together with your . . . -
Apr, 20 2024 — Yes. Even though Medicare plans sanctioned by the Centers for Medicare and Medicaid Services (CMS) are not allowed to accept new enrollment, Q1Medicare® shows “sanctioned” Medicare pl . . .
-
Apr, 20 2024 — 95% of your brand-name drug's retail cost is counted toward exiting the Donut Hole. If your monthly purchases of formulary medications consistently have a retail value of over $420, you will ex . . .
Most Viewed FAQs
-
Jan, 10 2024 — Your (1) Member ID number, (2) Rx BIN, (3) PCN, and (4) Group ID (or Rx Group) number are the four numbers that uniquely identify you and your Medicare Part D prescription drug plan - and these four n . . .
-
Feb, 02 2024 — You will receive a 75% discount on all formulary drugs if you reach the Donut Hole or Coverage Gap. Changes coming to the Medicare Part D Donut Hole. Spoiler Alert: In 2025, the Inflation Re . . .
-
 Apr, 20 2024 — Medicare Part D prescription drug plans provide insurance coverage for your out-patient prescription drugs - and works just like any other type of insurance:
(1) Monthly premium. You us . . .
Apr, 20 2024 — Medicare Part D prescription drug plans provide insurance coverage for your out-patient prescription drugs - and works just like any other type of insurance:
(1) Monthly premium. You us . . . -
Nov, 02 2023 — No. Medicare Advantage plans are not the same as Medicare Supplements or Medigap policies. And here are a few key differences between the plans: Medigap policy design Medica . . .
-
Apr, 20 2024 — You can drop, disenroll, or cancel your Medicare Part D plan or Medicare Advantage plan coverage during the annual Open Enrollment Period - or a Special Enrollment Period - or you can be involuntarily disenrolled from your plan.
-
May, 06 2024 — A Special Enrollment Period (SEP) allows a Medicare beneficiary to join, switch, or drop their Medicare Part D prescription drug plan (PDP) or Medicare Advantage plan (MA or MAPD) outside of the ann . . .
-
Mar, 06 2024 — The Qualified Medicare Beneficiary (QMB) program is one of four Medicare Savings Programs (QMB, SLMB, QI, and QDWI) established by Medicare to help low-income Medicare beneficiaries pay their Medicare . . .
-
May, 05 2024 — If you are eligible for Medicare and you don't have drug coverage through your employer, VA, or other source, additional prescription drug coverage is available to you through either: (1) a stand-a . . .
-
Apr, 20 2024 — If you did not enroll into a Medicare Part D prescription drug plan during your Initial Enrollment Period (IEP) and you did not have other creditable prescription drug coverage (like VA benefits or e . . .
-
Nov, 14 2023 — Yes. Medicare Part D prescription drug plans do cover the shingles vaccine (stand-alone Medicare Part D plans and Medicare Advantage plans that include drug coverage). And, beginning Janua . . .
-
Apr, 20 2024 — If you are paying IRMAA (the Income-Related Monthly Adjustment Amount), this means that, based on your income, you will pay higher premiums for your Medicare Part B and Medicare Part D coverage. As . . .
-
Jan, 21 2024 — To apply for the Medicare Part D Extra Help program: You can call the Social Security Administration about the Extra Help program at 1-800-772-1213, Monday through Friday between 7 am an . . .
-
Dec, 14 2023 — You have two options: You can select a new Medicare Part D plan that covers all of your medications. Medicaid and "Extra Help" recipients both receive a quarterly Special Enrollment Period and can . . .
-
Oct, 24 2023 — Yes. In 2024, over 3,000 counties (or ZIP code areas) include at least one Medicare Advantage plan with a Part B premium “Giveback” - 2024 Part B give-backs can range up to $164.90.
-
Jan, 30 2024 — TrOOP or your total out-of-pocket cost is the total amount you will spend in a year on your formulary drugs before exiting the Coverage Gap (or Donut Hole) and entering the Catastrophic Coverage of yo . . .
-
Jul, 26 2023 — No Medicare and Humana are not the same. Humana is one of the largest private insurance companies that provides, along with other products, Medicare Advantage plans and Medicare Part D prescripti . . .
-
Nov, 03 2023 — A Medicare Advantage MAPD (or MA-PD) plan includes Medicare Part D prescription drug coverage and a Medicare Advantage MA plan does not include drug coverage. Both MAs and MAPDs provide coverage of your Medicare Part A (in-patient care) and Medicare Part B (out-patient care).
-
 Apr, 20 2024 — If you are a Medicare beneficiary with higher annual earnings, you may be assessed an Income-Related Monthly Adjustment Amount (or IRMAA) which is an additional amount that you pay together with your . . .
Apr, 20 2024 — If you are a Medicare beneficiary with higher annual earnings, you may be assessed an Income-Related Monthly Adjustment Amount (or IRMAA) which is an additional amount that you pay together with your . . . -
Mar, 06 2024 — SLMB is one type of Medicare Savings Program for the "Specified Low - Income Medicare Beneficiary" and, according to the Centers for Medicare and Medicaid Services (CMS), SLMB is defined as: "A Medic . . .
-
 Nov, 05 2023 — Your Initial Coverage Limit (ICL) is the "boundary" between your Medicare Part D plan's Initial Coverage phase (where you and your drug plan share the cost of your drug purchases) and the Coverage Gap (where you receive a fixed 75% Donut Hole discount on formulary drugs
Nov, 05 2023 — Your Initial Coverage Limit (ICL) is the "boundary" between your Medicare Part D plan's Initial Coverage phase (where you and your drug plan share the cost of your drug purchases) and the Coverage Gap (where you receive a fixed 75% Donut Hole discount on formulary drugs
Browse FAQ Categories
Ask a Pharmacist*
Have questions about your medication?
» Answers to Your Medication Questions, Free!
Available Monday - Friday
8am to 5pm MST
8am to 5pm MST
*A free service included with your no cost drug discount card.
Q1 Quick Links
- Sign-up for our Medicare Part D Newsletter.
- PDP-Facts: 2024 Medicare Part D plan Facts & Figures
- 2024 PDP-Finder: Medicare Part D (Drug Only) Plan Finder
- PDP-Compare: 2023/2024 Medicare Part D plan changes
- 2024 MA-Finder: Medicare Advantage Plan Finder
- MA plan changes 2023 to 2024
- Drug Finder: 2024 Medicare Part D drug search
- Formulary Browser: View any 2024 Medicare plan's drug list
- 2024 Browse Drugs By Letter
- Guide to 2023/2024 Mailings from CMS, Social Security and Plans
- Out-of-Pocket Cost Calculator
- Q1Medicare FAQs: Most Read and Newest Questions & Answers
- Q1Medicare News: Latest Articles
- 2025 Medicare Part D Reminder Service
